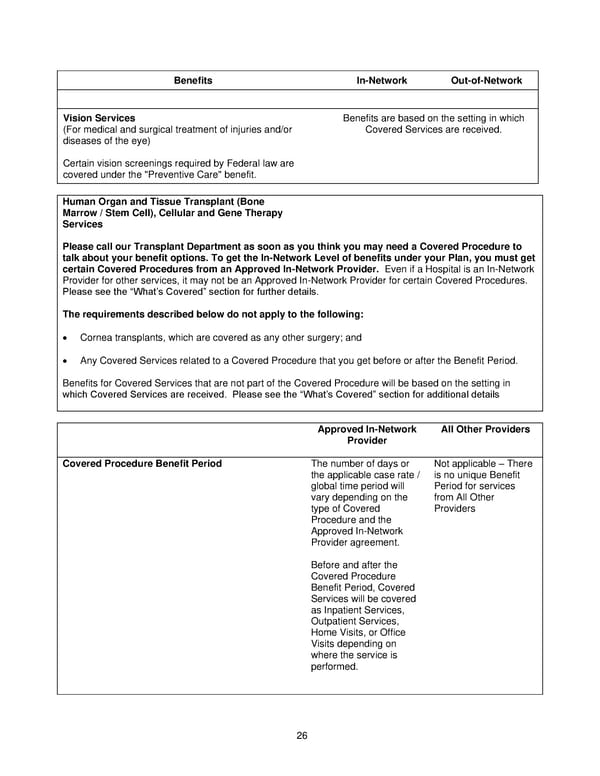
26 Benefits In-Network Out-of-Network Vision Services (For medical and surgical treatment of injuries and/or diseases of the eye) Certain vision screenings required by Federal law are covered under the "Preventive Care" benefit. Benefits are based on the setting in which Covered Services are received. Human Organ and Tissue Transplant (Bone Marrow / Stem Cell), Cellular and Gene Therapy Services Please call our Transplant Department as soon as you think you may need a Covered Procedure to talk about your benefit options. To get the In-Network Level of benefits under your Plan, you must get certain Covered Procedures from an Approved In-Network Provider. Even if a Hospital is an In-Network Provider for other services, it may not be an Approved In-Network Provider for certain Covered Procedures. Please see the “What’s Covered” section for further details. The requirements described below do not apply to the following: • Cornea transplants, which are covered as any other surgery; and • Any Covered Services related to a Covered Procedure that you get before or after the Benefit Period. Benefits for Covered Services that are not part of the Covered Procedure will be based on the setting in which Covered Services are received. Please see the “What’s Covered” section for additional details Approved In-Network Provider All Other Providers Covered Procedure Benefit Period The number of days or the applicable case rate / global time period will vary depending on the type of Covered Procedure and the Approved In-Network Provider agreement. Before and after the Covered Procedure Benefit Period, Covered Services will be covered as Inpatient Services, Outpatient Services, Home Visits, or Office Visits depending on where the service is performed. Not applicable – There is no unique Benefit Period for services from All Other Providers
 Anthem Blue Access PPO Option 23 with Rx Option T3 IN PPO Large 96R4 01 01 2025 L12026M001 L12026 English EOC CY Page 26 Page 28
Anthem Blue Access PPO Option 23 with Rx Option T3 IN PPO Large 96R4 01 01 2025 L12026M001 L12026 English EOC CY Page 26 Page 28