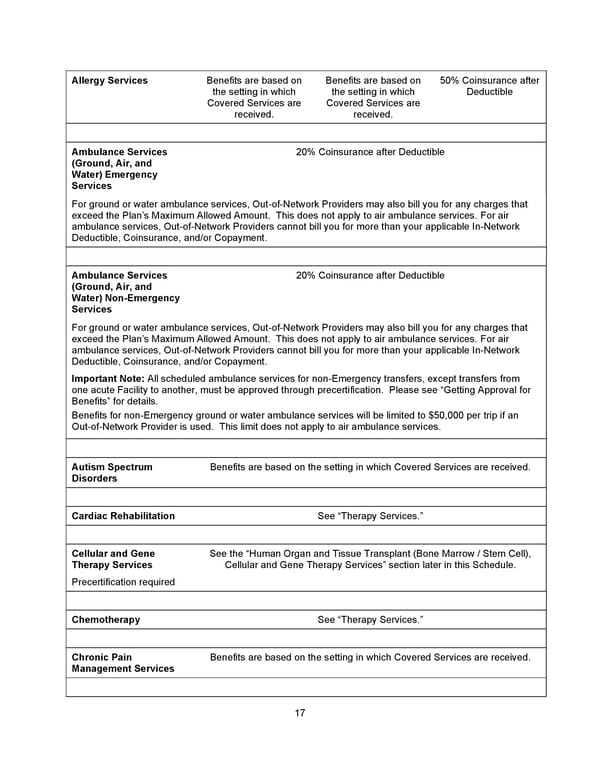
17 Allergy Services Benefits are based on the setting in which Covered Services are received. Benefits are based on the setting in which Covered Services are received. 50% Coinsurance after Deductible Ambulance Services (Ground, Air, and Water) Emergency Services 20% Coinsurance after Deductible For ground or water ambulance services, Out-of-Network Providers may also bill you for any charges that exceed the Plan’s Maximum Allowed Amount. This does not apply to air ambulance services. For air ambulance services, Out-of-Network Providers cannot bill you for more than your applicable In-Network Deductible, Coinsurance, and/or Copayment. Ambulance Services (Ground, Air, and Water) Non-Emergency Services 20% Coinsurance after Deductible For ground or water ambulance services, Out-of-Network Providers may also bill you for any charges that exceed the Plan’s Maximum Allowed Amount. This does not apply to air ambulance services. For air ambulance services, Out-of-Network Providers cannot bill you for more than your applicable In-Network Deductible, Coinsurance, and/or Copayment. Important Note: All scheduled ambulance services for non-Emergency transfers, except transfers from one acute Facility to another, must be approved through precertification. Please see “Getting Approval for Benefits” for details. Benefits for non-Emergency ground or water ambulance services will be limited to $50,000 per trip if an Out-of-Network Provider is used. This limit does not apply to air ambulance services. Autism Spectrum Disorders Benefits are based on the setting in which Covered Services are received. Cardiac Rehabilitation See “Therapy Services.” Cellular and Gene Therapy Services Precertification required See the “Human Organ and Tissue Transplant (Bone Marrow / Stem Cell), Cellular and Gene Therapy Services” section later in this Schedule. Chemotherapy See “Therapy Services.” Chronic Pain Management Services Benefits are based on the setting in which Covered Services are received.
 Benefit Booklet: Plan 2 Page 17 Page 19
Benefit Booklet: Plan 2 Page 17 Page 19