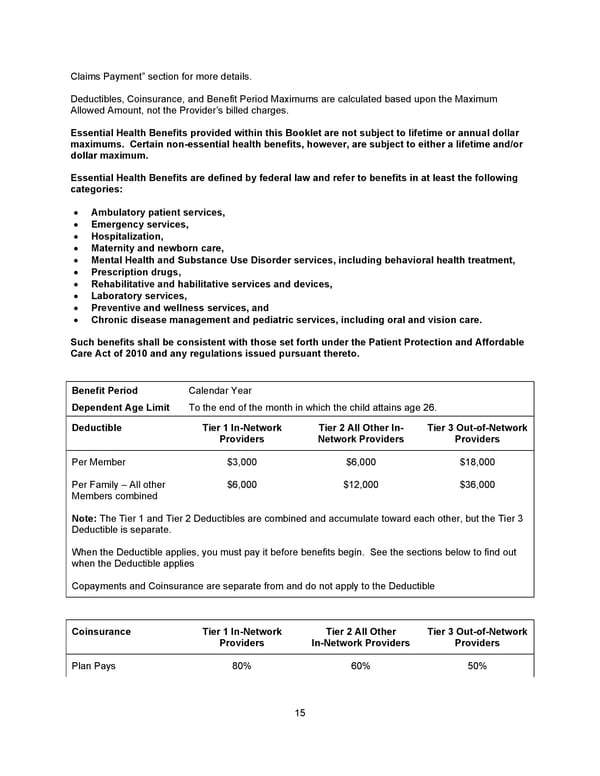
15 Claims Payment” section for more details. Deductibles, Coinsurance, and Benefit Period Maximums are calculated based upon the Maximum Allowed Amount, not the Provider’s billed charges. Essential Health Benefits provided within this Booklet are not subject to lifetime or annual dollar maximums. Certain non-essential health benefits, however, are subject to either a lifetime and/or dollar maximum. Essential Health Benefits are defined by federal law and refer to benefits in at least the following categories: • Ambulatory patient services, • Emergency services, • Hospitalization, • Maternity and newborn care, • Mental Health and Substance Use Disorder services, including behavioral health treatment, • Prescription drugs, • Rehabilitative and habilitative services and devices, • Laboratory services, • Preventive and wellness services, and • Chronic disease management and pediatric services, including oral and vision care. Such benefits shall be consistent with those set forth under the Patient Protection and Affordable Care Act of 2010 and any regulations issued pursuant thereto. Benefit Period Calendar Year Dependent Age Limit To the end of the month in which the child attains age 26. Deductible Tier 1 In-Network Providers Tier 2 All Other In- Network Providers Tier 3 Out-of-Network Providers Per Member $3,000 $6,000 $18,000 Per Family – All other Members combined $6,000 $12,000 $36,000 Note: The Tier 1 and Tier 2 Deductibles are combined and accumulate toward each other, but the Tier 3 Deductible is separate. When the Deductible applies, you must pay it before benefits begin. See the sections below to find out when the Deductible applies Copayments and Coinsurance are separate from and do not apply to the Deductible Coinsurance Tier 1 In-Network Providers Tier 2 All Other In-Network Providers Tier 3 Out-of-Network Providers Plan Pays 80% 60% 50%
 Benefit Booklet: Plan 2 Page 15 Page 17
Benefit Booklet: Plan 2 Page 15 Page 17