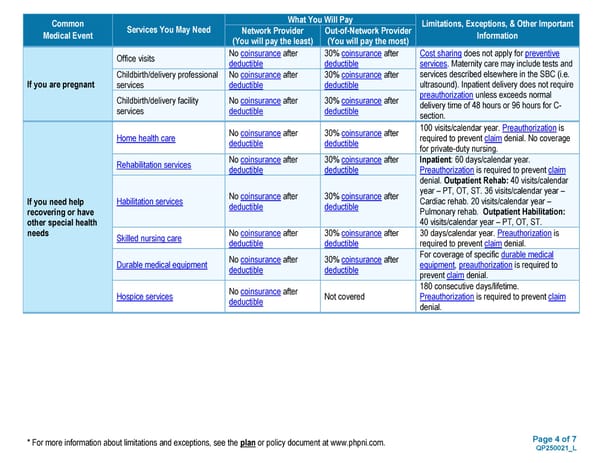
Page 4 of 7 QP250021_L * For more information about limitations and exceptions, see the plan or policy document at www.phpni.com. Common Medical Event Services You May Need What You Will Pay Limitations, Exceptions, & Other Important Information Network Provider (You will pay the least) Out-of-Network Provider (You will pay the most) If you are pregnant Office visits No coinsurance after deductible 30% coinsurance after deductible Cost sharing does not apply for preventive services. Maternity care may include tests and services described elsewhere in the SBC (i.e. ultrasound). Inpatient delivery does not require preauthorization unless exceeds normal delivery time of 48 hours or 96 hours for C- section. Childbirth/delivery professional services No coinsurance after deductible 30% coinsurance after deductible Childbirth/delivery facility services No coinsurance after deductible 30% coinsurance after deductible If you need help recovering or have other special health needs Home health care No coinsurance after deductible 30% coinsurance after deductible 100 visits/calendar year. Preauthorization is required to prevent claim denial. No coverage for private-duty nursing. Rehabilitation services No coinsurance after deductible 30% coinsurance after deductible Inpatient: 60 days/calendar year. Preauthorization is required to prevent claim denial. Outpatient Rehab: 40 visits/calendar year – PT, OT, ST. 36 visits/calendar year – Cardiac rehab. 20 visits/calendar year – Pulmonary rehab. Outpatient Habilitation: 40 visits/calendar year – PT, OT, ST. Habilitation services No coinsurance after deductible 30% coinsurance after deductible Skilled nursing care No coinsurance after deductible 30% coinsurance after deductible 30 days/calendar year. Preauthorization is required to prevent claim denial. Durable medical equipment No coinsurance after deductible 30% coinsurance after deductible For coverage of specific durable medical equipment, preauthorization is required to prevent claim denial. Hospice services No coinsurance after deductible Not covered 180 consecutive days/lifetime. Preauthorization is required to prevent claim denial.
 Plan 2 SBC Page 3 Page 5
Plan 2 SBC Page 3 Page 5