Plan 1 SBC
This document outlines the benefits, coverage, and cost-sharing details for the Physicians Health Plan, including deductibles, out-of-pocket expenses, and network provider information.
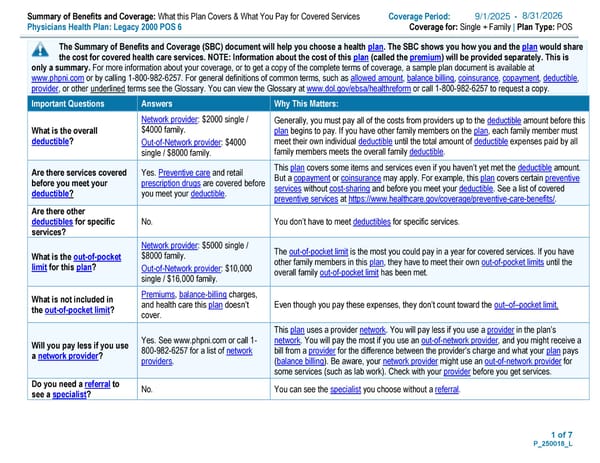
Summary of Benefits and Coverage: What this Plan Covers & What You Pay for Covered Services Coverage Period: - Physicians Health Plan: Legacy 2000 POS 6 Coverage for: Single + Family | Plan Type: POS 1 of 7 P_250018_L The Summary of Benefits and Coverage (SBC) document will help you choose a health plan. The SBC shows you how you and the plan would share the cost for covered health care services. NOTE: Information about the cost of this plan (called the premium) will be provided separately. This is only a summary. For more information about your coverage, or to get a copy of the complete terms of coverage, a sample plan document is available at www.phpni.com or by calling 1-800-982-6257. For general definitions of common terms, such as allowed amount, balance billing, coinsurance, copayment, deductible, provider, or other underlined terms see the Glossary. You can view the Glossary at www.dol.gov/ebsa/healthreform or call 1-800-982-6257 to request a copy. Important Questions Answers Why This Matters: What is the overall deductible? Network provider: $2000 single / $4000 family. Out-of-Network provider: $4000 single / $8000 family. Generally, you must pay all of the costs from providers up to the deductible amount before this plan begins to pay. If you have other family members on the plan, each family member must meet their own individual deductible until the total amount of deductible expenses paid by all family members meets the overall family deductible. Are there services covered before you meet your deductible? Yes. Preventive care and retail prescription drugs are covered before you meet your deductible. This plan covers some items and services even if you haven’t yet met the deductible amount. But a copayment or coinsurance may apply. For example, this plan covers certain preventive services without cost-sharing and before you meet your deductible. See a list of covered preventive services at https://www.healthcare.gov/coverage/preventive-care-benefits/. Are there other deductibles for specific services? No. You don’t have to meet deductibles for specific services. What is the out-of-pocket limit for this plan? Network provider: $5000 single / $8000 family. Out-of-Network provider: $10,000 single / $16,000 family. The out-of-pocket limit is the most you could pay in a year for covered services. If you have other family members in this plan, they have to meet their own out-of-pocket limits until the overall family out-of-pocket limit has been met. What is not included in the out-of-pocket limit? Premiums, balance-billing charges, and health care this plan doesn’t cover. Even though you pay these expenses, they don’t count toward the out–of–pocket limit. Will you pay less if you use a network provider? Yes. See www.phpni.com or call 1- 800-982-6257 for a list of network providers. This plan uses a provider network. You will pay less if you use a provider in the plan’s network. You will pay the most if you use an out-of-network provider, and you might receive a bill from a provider for the difference between the provider’s charge and what your plan pays (balance billing). Be aware, your network provider might use an out-of-network provider for some services (such as lab work). Check with your provider before you get services. Do you need a referral to see a specialist? No. You can see the specialist you choose without a referral. 9/1/2025 8/31/2026
 Plan 1 SBC Page 2
Plan 1 SBC Page 2