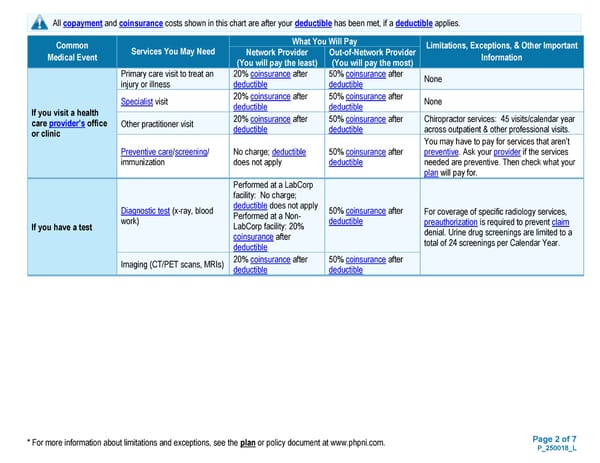
Page 2 of 7 P_250018_L * For more information about limitations and exceptions, see the plan or policy document at www.phpni.com. All copayment and coinsurance costs shown in this chart are after your deductible has been met, if a deductible applies. Common Medical Event Services You May Need What You Will Pay Limitations, Exceptions, & Other Important Information Network Provider (You will pay the least) Out-of-Network Provider (You will pay the most) If you visit a health care provider’s office or clinic Primary care visit to treat an injury or illness 20% coinsurance after deductible 50% coinsurance after deductible None Specialist visit 20% coinsurance after deductible 50% coinsurance after deductible None Other practitioner visit 20% coinsurance after deductible 50% coinsurance after deductible Chiropractor services: 45 visits/calendar year across outpatient & other professional visits. Preventive care/screening/ immunization No charge; deductible does not apply 50% coinsurance after deductible You may have to pay for services that aren’t preventive. Ask your provider if the services needed are preventive. Then check what your plan will pay for. If you have a test Diagnostic test (x-ray, blood work) Performed at a LabCorp facility: No charge; deductible does not apply Performed at a Non- LabCorp facility: 20% coinsurance after deductible 50% coinsurance after deductible For coverage of specific radiology services, preauthorization is required to prevent claim denial. Urine drug screenings are limited to a total of 24 screenings per Calendar Year. Imaging (CT/PET scans, MRIs) 20% coinsurance after deductible 50% coinsurance after deductible
 Plan 1 SBC Page 1 Page 3
Plan 1 SBC Page 1 Page 3